Article reviewed by:
Dr Helena Lee • Periodontist
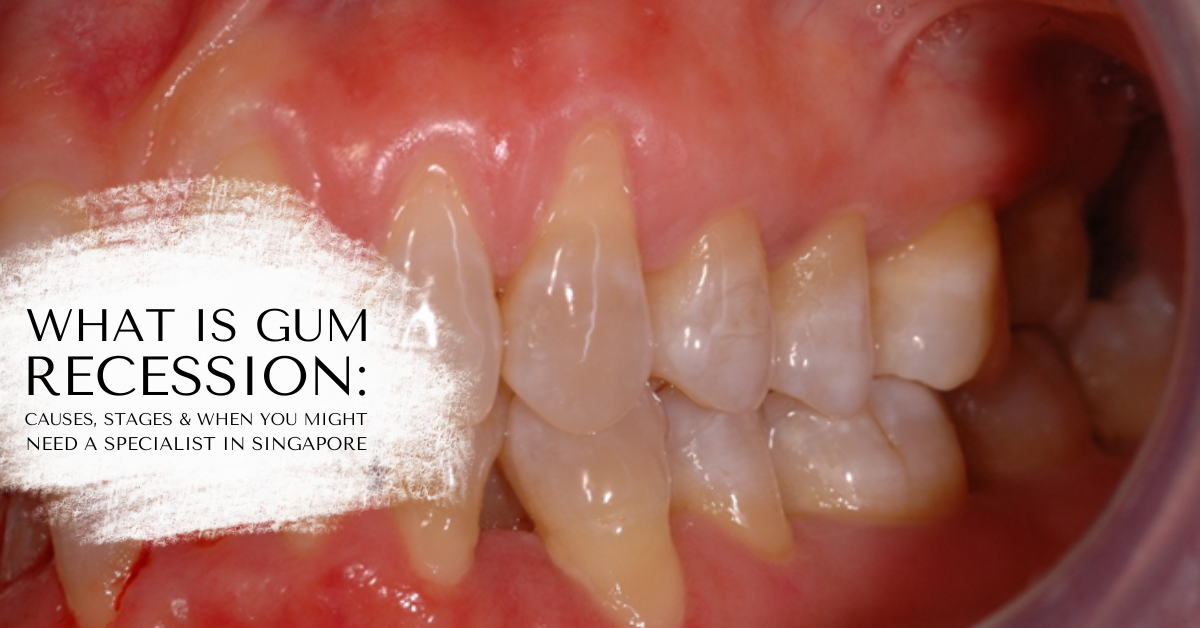
Have you noticed your teeth looking slightly longer than before, or felt increased sensitivity when eating or drinking? These are often early signs of gum recession, a condition in which gum tissue gradually recedes from the tooth surface, exposing areas that were previously covered.
For many people, this change happens slowly and without obvious discomfort at first. And because the progression is gradual, it is not always immediately noticeable until the effects become more visible or start to affect daily routines.
Why, you ask? Because as the protective gum layer recedes, the exposed root surface becomes more vulnerable to sensitivity, wear, and decay. As such, recognising any changes in your gums allows for timely assessment and helps guide the next steps in managing the condition.
Table of Contents
- What is Gum Recession
- What Causes Gum Recession
- Warning Signs of Receding Gums
- What Happens if Gum Recession is Left Untreated
- How to Fix Receding Gums?
- When to See a Periodontist for Gum Recession
- How to Prevent Gum Recession
- Speak to a Specialist at Specialist Dental Group
- Frequently Asked Questions
Key Takeaways
- Gum recession occurs when the gum tissue shifts away from the tooth, exposing the root surface.
- Early changes are often subtle and may only become noticeable over time.
- Seeking an assessment early can help manage progression and protect long-term gum health.
What is Gum Recession
Gum recession, also known as gingival recession according to SingHealth, describes a condition where the gum margin no longer sits at its usual position around the tooth. As the tissue recedes, the root surface becomes exposed. This can have an impact on a single tooth or multiple teeth, and the extent can vary from mild changes along the gum line to more advanced loss of tissue coverage. It is also important to note that once gum tissue has receded, it does not grow back on its own.
What Are the Stages of Gum Recession
The extent of gum recession can vary from subtle changes along the gum line to more advanced loss of tissue coverage. These stages are generally described based on how much of the root surface is exposed and how the gums respond over time.
- Early stage: Slight movement of the gum margin may be observed. The root surface is minimally exposed, and sensitivity may only be noticed occasionally.
- Moderate stage: The recession becomes more noticeable, with a greater portion of the root surface exposed. Sensitivity may occur more frequently.
- Advanced stage: A larger area of the root is exposed, and the gum line appears visibly uneven. Sensitivity may become more persistent, and there may be changes in how the teeth feel during daily activities.
- Severe stage: Extensive loss of gum tissue is present, with significant root exposure. At this stage, the supporting structures around the tooth may be affected, which can influence stability if not assessed and managed appropriately.
What Causes Gum Recession
While this condition can develop at any age, it is observed frequently in older adults. Certain factors may also increase the likelihood of developing gum recession, but it is often linked to a combination of factors rather than a single cause. In many cases, daily habits, underlying dental conditions, and individual susceptibility all play a role in how the gum line changes over time.
Common causes include:
- Plaque buildup: When not properly removed, plaque can harden along the gum line. This may lead to inflammation and, over time, contribute to changes in the supporting gum tissue.
- Gum disease (periodontal disease): Infection affecting the gums and surrounding structures can result in tissue breakdown and loss of attachment around the teeth.
- Brushing technique: Repeated brushing with excessive pressure or using a hard-bristle toothbrush may wear down the gum margin.
- Tooth alignment and orthodontic history: Teeth that are not positioned within the natural bone support, including after orthodontic movement in some cases, may be associated with thinner gum areas.
- Teeth grinding or clenching: Ongoing pressure on the teeth and surrounding tissues may affect how the gums respond over time.
- Tobacco use: Smoking or using tobacco can affect how the body responds to infection and healing, which may increase the likelihood of gum problems and make recovery slower once the gums are affected.
- Oral piercings: Lip or tongue piercings may repeatedly come into contact with the gum line, leading to localised tissue wear.
- Genetic factors: Some individuals naturally have thinner gum tissue, which may make them more susceptible to recession even with regular oral care.
Warning Signs of Receding Gums
Beyond visible changes, gum recession can also show up through how your teeth and gums feel. These signs may not always be constant, but they can become noticeable in specific situations.
Common signs to look out for include:
- Discomfort along the gum line: Certain areas may feel tender or uncomfortable, especially when brushing or flossing around the same spot.
- Sensitivity during dental visits: You may notice increased sensitivity during professional cleaning, particularly in areas where the gums have shifted.
- Food getting trapped more easily: Small gaps may form near the gum line, making it easier for food particles to collect in those areas.
- Teeth feeling less stable: In some cases, affected teeth may feel slightly different when biting or chewing.
- Localised changes in colour near the gum line: Areas closer to the gum margin may appear different in shade, which can become noticeable when compared to surrounding teeth.
If these changes start to affect your daily routine or become more consistent, it could mean that the condition has progressed beyond the early stage.
What Happens if Gum Recession is Left Untreated
When gum recession continues without being assessed, the changes do not remain limited to the gum line. Over time, the surrounding structures that support the teeth may also be affected.
Potential outcomes may include:
- Higher risk of decay along the root surface: The exposed root area does not have the same protective layer as the crown of the tooth, making it easier for decay to develop in those areas.
- Impact on tooth support in later stages: When the surrounding structures are affected over time, this may influence how stable the tooth feels during normal use.
- Tooth mobility and eventual loss: In later stages, changes in the supporting gum and bone structures may affect how firmly the tooth is held in place. This can lead to increased movement during biting or chewing, and if the condition progresses, it may affect the long-term retention of the tooth.
- Changes in jawbone support: Ongoing recession may be associated with a gradual reduction in the bone that supports the teeth. As this support changes, it can influence overall oral function and may also affect the way the lower part of the face appears over time.
How to Fix Receding Gums?

Management depends on the underlying cause and the extent of tissue involvement. In some cases, non-surgical care may be considered, while in other situations, it may involve procedures aimed at covering exposed areas or supporting the surrounding structures.
1. Non-Surgical Treatments
For cases where the condition is identified earlier, non-surgical approaches may be discussed. This often includes professional cleaning beneath the gumline to remove plaque or tartar that is hard to reach with regular brushing.
In certain situations, topical antibiotics may be applied to the gum area to manage bacterial activity associated with gum disease.
Other approaches may involve placing a tooth-coloured material over exposed root surfaces to reduce sensitivity and improve comfort. Where tooth positioning is a contributing factor, orthodontic care such as braces may be considered to adjust alignment, which may reduce strain on specific areas of the gum line over time.
2. Gum Graft Surgery
When a larger area of the root surface is exposed, a gum graft may be considered as part of receding gums treatment. This involves placing tissue over the affected area to cover the exposed root and support the gum margin.
The tissue is often taken from another area within the mouth or from a donor source, depending on the case. Once positioned, it is secured in place to allow it to integrate with the surrounding gum tissue. This approach is used to reduce sensitivity and provide additional coverage where needed.
3. Other Surgical Options
In some situations, other procedures may be discussed depending on the condition of the gums and surrounding bone. One approach involves lifting the gum tissue to allow access for cleaning deeper areas, before repositioning it closer to the tooth surface.
Where there has been a loss of supporting bone, materials may be placed to support the body’s natural healing response in that area. These procedures are selected based on the extent of the condition and the overall state of the surrounding structures.
When to See a Periodontist for Gum Recession
If changes along the gum line become noticeable or start affecting daily habits, it may be appropriate to seek a professional assessment. This includes situations where sensitivity becomes consistent, the gum line appears uneven, or areas near the root surface look exposed.
For those with braces or a history of orthodontic treatment, it can also be useful to have the gums reviewed if certain areas feel different when brushing or flossing. Early evaluation allows the condition to be monitored and managed based on how it is progressing, rather than waiting until the changes become more pronounced.
How to Prevent Gum Recession
While not all cases can be avoided, daily habits and regular care play a role in how the gum line changes over time.
- Use a soft-bristled toothbrush and apply controlled pressure when brushing, especially around the gum margin
- Clean between teeth consistently to reduce buildup in areas that are harder to reach
- Follow a regular dental visit schedule based on individual needs, including professional cleaning when advised
- Pay attention to brushing technique if you are wearing braces, as certain areas may require extra care
- Avoid habits that place repeated stress on the gums, such as aggressive brushing or using hard objects in the mouth
- Limit tobacco use, as it can affect how the gums respond to irritation and healing
Speak to a Specialist at Specialist Dental Group
If you have noticed ongoing changes along your gum line or have been advised to monitor certain areas, you may consider speaking with a periodontist for a closer assessment. At Specialist Dental Group, care is planned based on your condition, whether it involves monitoring, non-surgical care, or procedures such as receding gum treatments.
A consultation allows your gum health, tooth support, and contributing factors to be reviewed in detail. From there, a suitable approach for periodontal treatment can be discussed based on your needs and current condition.
Frequently Asked Questions
No, gum tissue does not regrow on its own once it has receded.
Fees can vary depending on the extent of the condition and the type of care required. A consultation is usually needed to assess your gums and provide an accurate estimate.
You may be referred to a periodontist if the condition involves deeper gum or bone structures, or if specialised care is required beyond general dental management.
Wish to learn more about treatment options for Gum Recession? Consult our dental specialists for personalised advice.
Drop us a text via the WhatsApp icon on the bottom right corner, enquire or call us at (65) 6733 7883.

Reviewed by Dr Helena Lee
Dr Helena Lee is a Periodontist with Specialist Dental Group®. She received her speciality training from the University of London. She is a fellow of the Academy of Medicine, Singapore and a member of Society of Periodontology, Singapore. Dr Lee has a special interest in the treatment and prevention of periodontal disease, gingival plastic surgery, soft and hard tissue grafting and dental implants.
Disclaimer
This article has been medically reviewed by a specialist from Specialist Dental Group and is intended for general educational and informational purposes only. It should not be taken as a substitute for personalised dental advice, diagnosis, or treatment. Patients should consult a qualified dentist or dental specialist before making decisions about any procedure or treatment plan. Treatment recommendations should always be based on the patient’s individual clinical condition, and results may vary.